A bunion is a bony bump that forms at the base of the big toe, causing the toe to angle toward the second toe. This misalignment leads to pain, swelling, and difficulty in finding comfortable shoes. Bunions are often caused by a combination of factors, including genetics, abnormal foot mechanics, and wearing tight, ill-fitting shoes that put excessive pressure on the toes. Over time, the pressure can force the joint to shift, resulting in the formation of the bony protrusion. The severity of bunions can vary, with mild cases causing minimal discomfort, while severe cases may lead to significant pain and difficulty walking. In more advanced stages, the affected toe may become rigid and inflamed. Relief options range from conservative measures such as wearing supportive shoes and using padding, to surgical intervention in extreme cases where pain and deformity are unmanageable. If you have a bunion, it is suggested that you are under the care of a podiatrist who can monitor its growth, and offer appropriate treatment solutions.
If you are suffering from bunions, contact Donald Manger, DPM of Associated Podiatric Physicians, PA. Our doctor can provide the care you need to keep you pain-free and on your feet.
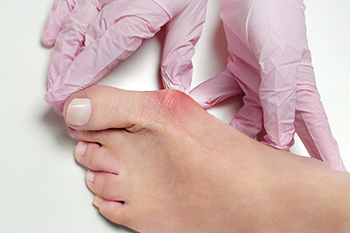
What Is a Bunion?
A bunion is formed of swollen tissue or an enlargement of boney growth, usually located at the base joint of the toe that connects to the foot. The swelling occurs due to the bones in the big toe shifting inward, which impacts the other toes of the foot. This causes the area around the base of the big toe to become inflamed and painful.
Why Do Bunions Form?
Genetics – Susceptibility to bunions are often hereditary
Stress on the feet – Poorly fitted and uncomfortable footwear that places stress on feet, such as heels, can worsen existing bunions
How Are Bunions Diagnosed?
Doctors often perform two tests – blood tests and x-rays – when trying to diagnose bunions, especially in the early stages of development. Blood tests help determine if the foot pain is being caused by something else, such as arthritis, while x-rays provide a clear picture of your bone structure to your doctor.
How Are Bunions Treated?
- Refrain from wearing heels or similar shoes that cause discomfort
- Select wider shoes that can provide more comfort and reduce pain
- Anti-inflammatory and pain management drugs
- Orthotics or foot inserts
- Surgery
If you have any questions, please feel free to contact our office located in Hamilton Township, NJ . We offer the newest diagnostic and treatment technologies for all your foot care needs.

A broken ankle occurs when one or more bones in the joint crack or break due to trauma, such as a fall, sports injury, or car accident. Symptoms typically include severe pain, swelling, bruising, and difficulty walking or bearing weight. The ankle may look deformed or feel unstable, depending on the severity of the break. A podiatrist diagnoses a broken ankle through a physical exam and imaging tests like X-rays or CT scans to determine the exact location and how serious the fracture is. Treatment varies based on the type of break. Minor fractures may only require a cast or boot to immobilize the ankle, while more severe breaks could need surgery to realign and stabilize the bones with screws or plates. If you suspect you have an ankle fracture, it is suggested that you promptly see a podiatrist to ensure proper healing and recovery.
Broken ankles need immediate treatment. If you are seeking treatment, contact Donald Manger, DPM from Associated Podiatric Physicians, PA. Our doctor can provide the care you need to keep you pain-free and on your feet.
Broken Ankles
A broken ankle is experienced when a person fractures their tibia or fibula in the lower leg and ankle area. Both of these bones are attached at the bottom of the leg and combine to form what we know to be our ankle.
When a physician is referring to a break of the ankle, he or she is usually referring to a break in the area where the tibia and fibula are joined to create our ankle joint. Ankles are more prone to fractures because the ankle is an area that suffers a lot of pressure and stress. There are some obvious signs when a person experiences a fractured ankle, and the following symptoms may be present.
Symptoms of a Fractured Ankle
- Excessive pain when the area is touched or when any pressure is placed on the ankle
- Swelling around the area
- Bruising of the area
- Area appears to be deformed
If you suspect an ankle fracture, it is recommended to seek treatment as soon as possible. The sooner you have your podiatrist diagnose the fracture, the quicker you’ll be on the way towards recovery.
If you have any questions, please feel free to contact our office located in Hamilton Township, NJ . We offer the newest diagnostic and treatment technologies for all your foot care needs.

Bumps on the bottom of the foot, such as plantar fibromas, are often benign growths that develop in the tissue beneath the skin, known as the plantar fascia. However, other conditions like calluses or bone spurs can also cause similar lumps. Plantar fibromas are firm, rubbery lumps that can vary in size and may cause discomfort or pain, especially when walking or standing. The exact cause of plantar fibromas is unclear, but factors like genetics, trauma, or repetitive stress on the feet can contribute. Symptoms include localized pain, swelling, and sometimes a noticeable lump under the arch of the foot. In some cases, the fibroma or lump can interfere with movement and cause difficulty with footwear. Treatment options range from conservative methods, such as stretching exercises, orthotic insoles, and corticosteroid injections, to surgical removal, in more severe cases. A podiatrist can provide a thorough diagnosis and tailored treatment plan to relieve discomfort and prevent further complications. If you have this condition, it is suggested that you schedule an appointment with a podiatrist.
Foot Pain
Foot pain can be extremely painful and debilitating. If you have a foot pain, consult with Donald Manger, DPM from Associated Podiatric Physicians, PA. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
Causes
Foot pain is a very broad condition that could be caused by one or more ailments. The most common include:
- Bunions
- Hammertoes
- Plantar Fasciitis
- Bone Spurs
- Corns
- Tarsal Tunnel Syndrome
- Ingrown Toenails
- Arthritis (such as Gout, Rheumatoid, and Osteoarthritis)
- Flat Feet
- Injury (from stress fractures, broken toe, foot, ankle, Achilles tendon ruptures, and sprains)
- And more
Diagnosis
To figure out the cause of foot pain, podiatrists utilize several different methods. This can range from simple visual inspections and sensation tests to X-rays and MRI scans. Prior medical history, family medical history, and any recent physical traumatic events will all be taken into consideration for a proper diagnosis.
Treatment
Treatment depends upon the cause of the foot pain. Whether it is resting, staying off the foot, or having surgery; podiatrists have a number of treatment options available for foot pain.
If you have any questions, please feel free to contact our office located in Hamilton Township, NJ . We offer the newest diagnostic and treatment technologies for all your foot care needs.